
REVIEW ARTICLE
HAEMATINICS FOR ANAEMIA IN THE ELDERLY
CASE HISTORY 3
Key feature: Routine folate therapy for normochromic normocytic anaemia with leucopenia.
Madam C is a 68-year-old lady who is on regular follow up for hypertension, diabetes and hyperlipidaemia at a specialist clinic in a general hospital. She was found to have pallor eight years ago at one of the routine consultations, but she denied ever having any symptoms related to anaemia. Her yearly blood test results consistently showed normochromic, normocytic anaemia of around 10 g/dL and a leucopenia of around 3.4 x 109/L. Platelet count is usually at the low normal range of about 170 x 109/L. Full blood picture (FBP) did not show any morphological changes in the red and white blood cells (WBC) and platelets. Renal and liver function tests, serum calcium and phosphates, random blood sugar, HbA1c, cholesterol level and urine tests were all within normal range. X-rays of chest and lumbosacral spine were normal except for minor degenerative changes.
A full workout for multiple myeloma was performed on her five years ago but results of all the relevant tests were negative for this medical condition. She was treated with daily folic acid for past two years without any improvement in the FBC indices. Lately, a new physician took over the practice and suggested that her persistent mild anaemia and leucopenia could be due to myelodysplastic syndrome and she may require a bone marrow biopsy to confirm the diagnosis. Patient is very worried as she was told that myelodysplastic syndrome is a pre-cursor to myeloid leukemia. She consults you for a second opinion.
Questions:
- Do you agree with this new physician’s suggestion?
- What further simple tests can you recommend her to do before she is subjected to the invasive procedure of bone marrow biopsy?
- Results of the tests you recommended have come back positive, what is your treatment plan?
- What would be the clinical implication of long term folic acid therapy without being aware of the correct diagnosis in this case?
Commentary:
A well-known etiology of anaemia that increases with age is myelodysplasia (MDS). Occult MDS may be an important cause of "unexplained" anaemias in the elderly.22 This syndrome, thought in the past to represent pre-leukaemia, is characterized by a defect in the development of one of the marrow cell lines, limiting the release of functioning cells. Myelodysplastic syndrome should be a diagnostic consideration when white cell or platelet abnormalities accompany the anaemia. The diagnosis of this syndrome is usually made by bone marrow biopsy.18
On routine questioning, it was discovered that Madam C, though not a pure vegetarian, eats mostly vegetables and occasionally fish, but has practically excluded meat from her diet for many years. Laboratory workouts for nutritional deficiency anaemia were not done before. So far, peripheral blood film done 3-4 times in the past did not suggest morphological changes in the blood cells.
Nutritional deficiency anaemias need to be considered and investigated for in this case. Nutritional deficiency anaemias are easily diagnosed, treatments are simple, inexpensive and effective. Laboratory workout for iron, vitamin B12 and folate should be given priority to bone marrow biopsy. Red cell folate concentration is more reliable than the serum level and should be considered. Serum homocysteine (HC) level is elevated in 90% of patients with folate deficiency23 and can be useful for detecting folate deficiency in patients with low-normal serum folate levels. If methylmalonic acid (MMA) level is also elevated, vitamin B12 deficiency must be considered even if serum vitamin B12 is within low-normal range.23
For Madam C, further blood tests indicated low serum vitamin B12 of 78 pmol/L while all other parameters for iron and folate were within normal limits.
Vitamin B12 deficiency is treated with vitamin B12 supplementation, parenterally or orally. The intramuscular dose is 1,000 µg, often given daily for one week to build up stores, then weekly for one month and then monthly thereafter. A response to therapy, characterized by an increase in reticulocytosis, often occurs within a week of the initiation of vitamin B12 therapy.18 In the elderly, the main causes of cobalamin deficiency are pernicious anaemia (20-30%) and food-cobalamin malabsorption (50-70%).24 Food-cobalamin malabsorption syndrome, which has only recently been identified, is a disorder characterized by the inability to release cobalamin from food or its binding proteins.25 Absorption of ‘unbound’ cobalamin (free crystalline) is normal. Oral cobalamin of 1,000 µg daily can be used to treat this condition.
Some facts to note about vitamin B12 deficiency:
- Signs of vitamin B12 deficiency are not reliably present in the elderly. Only about 60% of patients with vitamin B12 deficiency are anaemic.26
- Neurologic symptoms of B12 deficiency can develop before the patient becomes anaemic.27
- Although anaemia due to vitamin B12 deficiency is usually macrocytic and megaloblastic, it can be normocytic or even microcytic if there is concomitant iron deficiency or beta thalassaemia trait.
- Serum vitamin B12 levels do not reliably reflect vitamin B12 deficiency. Up to 30% of patients with low-normal serum vitamin B12 levels have anaemia and neurologic disease.28
- Serum MMA and HC levels are sensitive for detecting subclinical vitamin B12 and folate deficiency, virtually excluding vitamin B12 deficiency when they are normal.23
- The symptoms of folate deficiency are nearly indistinguishable from those of vitamin B12 deficiency. Elderly individuals are frequently vitamin takers and food is often fortified with folic acid. Thus, megaloblastic anaemias due to folate deficiency in the elderly appear to be rare; when they do occur, they are often related to alcohol abuse.22
- Identification of vitamin B12 deficiency is important: anaemia secondary to vitamin B12 deficiency may improve with folate therapy, but folate therapy does not reverse the neurological damage caused by vitamin B12 deficiency. Progression of neurological damage may be masked by improvement of anaemia if concomitant vitamin B12 deficiency is not corrected accordingly.
CASE HISTORY 4
Key feature: Routine iron therapy for normochromic normocytic anaemia in advanced malignancy.
Mr D, a 75-year-old man, was diagnosed with fourth stage moderately differentiated squamous cell carcinoma of the lungs. He has completed a course of radiotherapy and is currently complaining of giddiness, breathlessness on walking, palpitation and lethargy. He is alert, mobile, though not as active as before and his general condition is fairly satisfactory except for pallor and recent loss of body weight of about 3 kg, leaving him to be at his current 56 kg status. Result of his Hb level has come back as 7 g/dL; white cell and platelet counts are within low normal range. Serum calcium is within high normal range, liver and renal function tests and blood sugar are normal. Mr D was treated with ferrous fumarate 200 mg bd. and folate 5 mg daily for past two months without much improvement.
Questions:
- Do you think oral haematinics will help to relieve Mr D’s complaints of giddiness, breathlessness, palpitation and lethargy?
- What would be the most appropriate treatment for his anaemia at this stage?
Commentary:
In late stage malignancy, symptoms attributable to the anaemia may also be due to underlying malignancy, chronic inflammation, blood loss, bone marrow suppression or invasion, malnutrition, or haemolysis.29
In anaemia of chronic disease, there is an impaired ability to use the iron stored in the reticuloendothelial system. Iron is not available for erythropoiesis, which is the similarity between anaemia of chronic disease and IDA. However, the iron stores are normal or increased, erythrocytes are usually normochromic and normocytic, although one third of patients may have microcytosis. TIBC is usually below normal because iron stores are elevated and as an acute-phase reactant, transferrin is reduced in the presence of acute and chronic stress.30 Serum ferritin level is the most useful test, differentiating anaemia of chronic disease from IDA in 70% of patients.31 (Table 1).
Iron supplementation provides no benefit in patients with anaemia of chronic disease and if taken when body iron stores are saturated, iron overload may occur with resultant detrimental consequences.32 Hence, oral haematinics would not be helpful in alleviating Mr D’s complaints.
Early studies showed that erythropoietin reduced the need for transfusions, raised Hb level and improved quality of life in patients receiving cancer treatment.33 However, a subsequent study was terminated early due to an increased number of thrombotic events in the treatment arm34 and another showed an increased risk of adverse events, including mortality when Hb was raised to above 11.3 g/dL.35 Other disadvantages include its cost, its efficacy in only some patients and the 4-8 weeks delay before maximum benefit is achieved. Currently erythropoietin is not recommended as a treatment for anaemia in palliative care.36
S Tanneberger et al. concluded that blood transfusion does offer prompt symptom relief and improvement of well-being in anaemic patients with terminal malignancy.37 RBC transfusions are commonly used as a treatment, whatever the cause of the anaemia, especially when anaemia is symptomatic and the Hb drops below 8 g/dL.36 Decision to use blood transfusion to palliate symptoms of anaemia requires a pragmatic approach. It means taking into consideration the severity of symptoms, Hb level, possible burden of cost and side effects, actual prognosis, general well being of patients, other organ dysfunction, onset and duration of therapeutic effects, as well as patient’s wish and competency to make a valid decision.
CASE HISTORY 5
Key feature: Routine iron therapy for normochromic normocytic anaemia at the end-of-life.
Mr E, who is an 88-year-old man living in a residential home for the aged, has multiple joint deformities and contractions with generalised muscle wasting. He has been confined to bed for past two years and has an extensive deep decubitus ulcer over the lumbosacral area. He has diabetes mellitus (DM) currently controlled with metformin 500 mg bd. He has past history of recurrent strokes and mild renal and liver impairment. He is semiconscious, able to respond to calls at times but more often remains unresponsive.
For the past three days, Mr E was having spiking fever temporarily controlled with paracetamol. You noticed that he looked extremely pale and his left knee joint was grossly swollen and inflammed. There was moderate joint effusion with marked tenderness on palpation as deduced from his facial expressions of pain. You checked through his medical record. He has normochromic normocytic anaemia of around 8 g/dL for years and has been treated regularly with oral ferrous fumarate 200 mg daily and folate 5 mg daily for years. You explained that hospitalization was necessary for treatment of his pyogenic arthritis, decubitus ulcer, control of blood sugar, anaemia and possible septicaemia. But his relatives and residential home carers did not agree to any more active medical interventions in the hospital. They requested you to do whatever you can to ease his sufferings at home.
Questions:
- Do you think that those years of iron and folic acid therapy was useful for Mr E?
- What better option was there to treat his anaemia in this clinical situation?
- How would you respond to the relatives’ and carers’ decisions of not sending him to the hospital for further active medical interventions?
Commentary:
For similar reasons as in Case 4, years of iron therapy provided no benefit but only increased the total body iron stores. Use of RBC transfusion to provide prompt relief of anaemia is also indicated here. However, in view of Mr E’s poor general condition, multiple organ dysfunction and bleak prognosis, the risks of blood transfusion outweigh the benefits. Mr E’s relatives and carers were requesting for limited treatment plan so as not to prolong his sufferings. When further treatments and investigations are futile in providing cure or comfort, but instead will incur more sufferings, it is justified to withhold them. If Mr E had provided treatment directives, a living will or power of attorney to make decision on his behalf earlier on, it would have been easier to apply this concept of limited treatment plan or DNR (Do Not Resuscitate). Limited treatment plan does not mean no more care for the patient. Palliative care could still be given in the form of good basic nursing care and psychological support for patients and carers.
CONCLUSION
Iron therapy in the absence of iron deficiency may be detrimental to the health of the elderly. Anaemias in the elderly require further investigations and must not simply be considered as part of ageing. Factors that need to be considered in the treatment plan includes the underlying causes of the anaemia, Hb level, symptoms, concomitant illnesses, physical status of patients, prognosis, cost and burden of treatment and whether for curative or palliative intention.
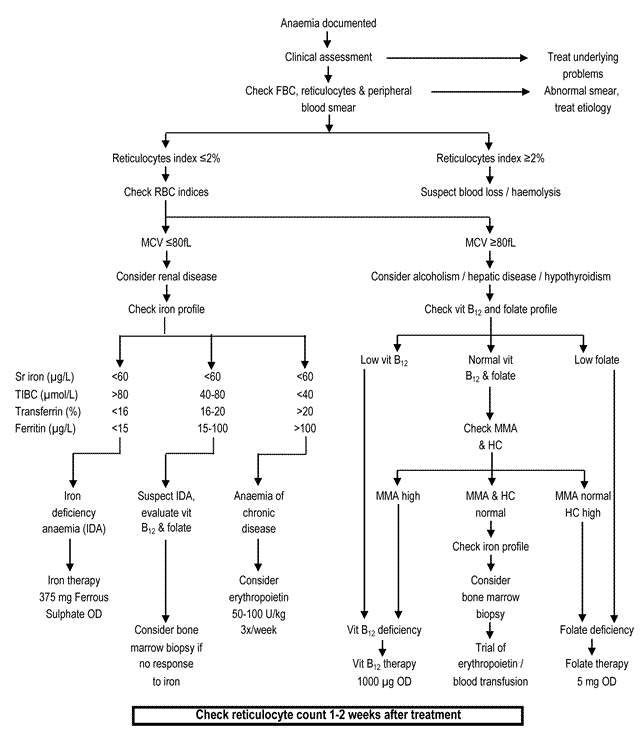
Figure 1 provides a flow chart in the assessments of common causes of anaemia in the elderly.
Figure 1: Management of anaemia in the elderly18
REFERENCES
- Guralnik JM, Eisenstaedt RS, Ferrucci L, et al. Prevalence of anemia in persons 65 years and older in the United States: evidence for a high rate of unexplained anemia. Blood. 2004;104(8):2263-8. [PubMed] [Full text]
- Zablocki E. Some U.S. elderly take unnecessary iron supplements. WebMD Health News. 2001. [Online] [Full text]
- Fleming DJ, Jacques PF, Tucker KL, et al. Iron status of the free-living, elderly Framingham Heart Study cohort: an iron-replete population with a high prevalence of elevated iron stores. Am J Clin Nutr. 2001;73(3):638-46. [PubMed] [Full text]
- Muretto P, Angelucci E, Lucarelli G. Reversibility of cirrhosis in patients cured of thalassemia by bone marrow transplantation. Ann Intern Med. 2002;136(9):667-72. [PubMed] [Full text]
- Klipstein-Grobusch K, Koster JF, Grobbee DE, et al. Serum ferritin and risk of myocardial infarction in the elderly: the Rotterdam Study. Am J Clin Nutr. 1999;69(6):1231-6. [PubMed] [Full text]
- Jiang R, Manson JE, Meigs JB, et al. Body iron stores in relation to risk of type 2 diabetes in apparently healthy women. JAMA. 2004;291(6):711-7. [PubMed] [Full text]
- Montgomery EB Jr. Heavy metals and the etiology of Parkinson’s disease and other movement disorders. Toxicology. 1995;97(1-3):3-9. [PubMed]
- de Sousa M, Porto G. The immunological system in hemochromatosis. J Hepatol. 1998;28(Suppl 1):1-7. [PubMed]
- Herbert V, Shaw S, Jayatilleke E, et al. Most free-radical injury is iron related: it is promoted by iron, hemin, holoferritin and vitamin c, and inhibited by desferoxamine and apoferritin. Stem Cells. 1994;12(3):289-303. [PubMed]
- Smith MA, Harris PL, Sayre LM, et al. Iron accumulation in Alzheimer disease is a source of redox-generated free radicals. Proc Natl Acad Sci USA. 1997;94(18):9866-8. [PubMed] [Full text]
- Nelson RL. Iron and colorectal cancer risk: human studies. Nutr Rev. 2001;59(5):140-8. [PubMed]
- Salonen JT, et al. The role of iron in diabetes and coronary heart disease. Metals Ions Bio Med. 1998;485-490.
- de Valk B, Marx JJ. Iron, atherosclerosis, and ischemic heart disease. Arch Intern Med. 1999;159(14):1542-8. [PubMed][Full text]
- Goddard AF, James MW, McIntyre AS, et al. Guidelines for the management of iron deficiency anaemia. Gut. 2000;46:(iv)1-5. [PubMed]
- Mukhopadhyay D, Mohanaruban K. Iron deficiency anaemia in older people: investigation, management and treatment. Age Ageing. 2002;31(2):87-91.[PubMed] [Full text]
- Murphy PT, Hutchinson RM. Identification and treatment of anaemia in older patients. Drugs Aging. 1994;4(2):113-27. [PubMed]
- Guyatt GH, Oxman AD, Ali M, et al. Laboratory diagnosis of iron-deficiency anaemia: an overview. J Gen Intern Med. 1992;7(2):145-53. [PubMed]
- Smith DL. Anemia in the elderly. Am Fam Physician. 2000;62(7):1565-72. [PubMed]
- British Columbia Medical Association Guidelines and Protocols Advisory Committee. Iron Deficiency - Investigation and Management. 2010. [Online] [Full text]
- Rimon E, Kagansky N, Kagansky M, et al. Are we giving too much iron? Low-dose iron therapy is effective in octogenarians. Am J Med. 2005;118(10):1142-7. [PubMed] [Full text]
- Linker C A. Blood - Anaemias. In: Current medical diagnosis and treatment. Edited by Tierney LM, McPhee SJ & Papadakis MA. 47th ed. The McGraw Hills Companies Inc USA; 1998. p. 422-37.
- Guralnik JM, Ershler WB, Schrier SL, et al. Anemia in the elderly: a public health crisis in hematology. Hematology. 2005. [Online] [Full text]
- Savage DG, Lindenbaum J, Stabler SP, et al. Sensitivity of serum methylmalonic acid and total homocysteine determinations for diagnosing cobalamin and folate deficiencies. Am J Med. 1994; 96(3):239-46. [PubMed]
- Andrès E, Goichot B, Schlienger JL. Food cobalamin malabsorption: a usual cause of vitamin B12 deficiency. Arch Intern Med. 2000;160(13):2061-2.[PubMed]
- Dawson DW, Gozzard DI, Lewis MJ. Protein-bound vitamin B12 absorption test. J Clin Pathol. 1988;41(4):478-9. [PubMed] [Full text]
- Joosten E, Ghesquiere B, Linthoudt H, et al. Upper and lower gastrointestinal evaluation of elderly inpatients who are iron deficient. Am J Med. 1999;107(1):24-9. [PubMed]
- Nexo E, Hansen M, Rasmussen K, et al. How to diagnose cobalamin deficiency. Scand J Clin Lab Invest Suppl. 1994; 219:61-76. [PubMed]
- Stabler SP. Vitamin B12 deficiency in older people: improving diagnosis and preventing disability. J Am Geriatr Soc. 1998;46(10):1317-9. [PubMed]
- Turner RA. Haematological aspects. In: Doyle D, Hanks G, Cherny N, editors. 2nd ed. Oxford Textbook of Palliative Medicine. Oxford University Press Inc. New York; 1998. p. 769-76.
- Lipschitz DA. The anemia of chronic disease. J Am Geriatr Soc. 1990;38(11):1258-64. [PubMed]
- Kis AM, Carnes M. Detecting iron deficiency in anemic patients with concomitant medical problems. J Gen Intern Med. 1998;13(7):455-61. [PubMed] [Full text]
- Weiss G, Goodnough LT. Anaemia of chronic disease. N Engl J Med. 2005;352(10):1011-23. [PubMed]
- Davis MP. Hematology in palliative medicine. Am J Hosp Palliat Care. 2004;21(6):445-54. [PubMed]
- Rosenzweig MQ, Bender CM, Lucke JP, et al. The decision to prematurely terminate a trial of R-HuEPO due to thrombotic events. J Pain Symptom Manage. 2004;27(2):185-90. [PubMed] [Full text]
- Singh AK, Szczech L, Tang KL, et al. Correction of anemia with epoeitin alfa in chronic kidney disease. N Engl J Med. 2006; 355(20):2085-98. [PubMed] [Full text]
- Hirst B. Management of anaemia in palliative care. 2009. [Online] [Full text]
- Tanneberger S, Melilli G, Strocchi E, et al. Use of red blood cell transfusion in palliative care services: is it still up to date or is cancer-related anaemia controlled better with erythropoietic agents? Ann Oncol. 2004;15(5):839-40. [PubMed] [Full text]
- Daly MP. Anemia in the elderly. Am Fam Physician. 1989;39(3):129-36. [PubMed]
- Joosten E, Pelemans W, Hiele M, et al. Prevalence and causes of anaemia in a geriatric hospitalized population. Gerontology. 1992;38(1-2):111-7. [PubMed]
- Kikuchi M, Inagaki T, Shinagawa N. Five-year survival of older people with anemia: variation with hemoglobin concentration. J Am Geriatr Soc. 2001;49(9):1226-8. [PubMed]
